Are Nootropic Supplements Safe? Complete Safety Guide

Nootropic safety depends entirely on which specific compound you're considering, prescription stimulants carry cardiovascular risks requiring medical supervision, while established supplements like omega-3s and caffeine have decades of safety data at recommended doses. The term "nootropics" encompasses everything from FDA-approved medications to unregulated synthetic compounds, each with vastly different risk profiles. Your individual health status, current medications, and proper dosing practices matter more than blanket claims about nootropic safety as a category.
Table of Contents
- Understanding Nootropic Safety: What You Need to Know First
- The Safety Spectrum: From FDA-Approved to Unregulated
- Why Age Matters: Safety Considerations for Adults 55+
- Prescription Nootropics: FDA-Regulated Cognitive Enhancers
- Medications for Cognitive Decline: Safety Track Record
- Stimulant Nootropics: Higher Risk Profile
- Over-the-Counter Nootropic Supplements: What Science Says About Safety
- Natural Doesn't Always Mean Safe: Common Misconceptions
- The Most Studied Supplements: Safety Evidence
- Supplements with Limited Safety Data
- Critical Safety Risks: Drug Interactions and Contraindications
- Cardiovascular Medication Interactions
- Neurological and Psychiatric Medication Interactions
- When Nootropics Are Not Safe: Medical Contraindications
- Quality and Purity: The Hidden Safety Issue in Supplements
- Third-Party Testing: Your Safety Net
- Standardization and Bioavailability Concerns
- Storage and Expiration: Often Ignored Safety Factors
- Side Effects and How to Minimize Risks
- Common Side Effects by Category
- The Importance of Cycling and Tolerance
- Start Low, Go Slow: Dose Escalation Strategy
- Making a Safe Decision: Your Nootropic Safety Checklist
- Before Starting Any Nootropic
- Monitoring and Adjustment
- Red Flags: When to Avoid a Nootropic
Understanding Nootropic Safety: What You Need to Know First
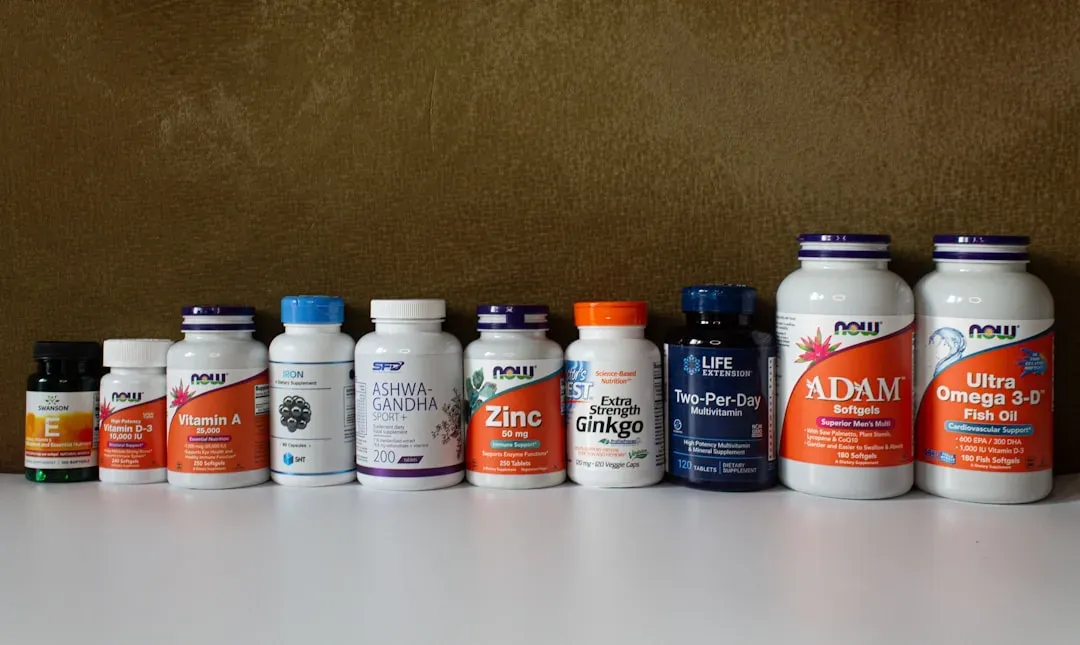
The safety question requires understanding that nootropics exist on a spectrum rather than as a single category. On one end sit prescription medications like donepezil (Aricept) and modafinil (Provigil), which undergo rigorous FDA testing before approval. These drugs have documented side effect profiles, established dosing guidelines, and contraindications based on thousands of patient-years of data.
Safety Profile Comparison: Nootropic Categories
| Nootropic Category | Regulatory Status | Safety Evidence | Typical Risk Level | Key Considerations |
|---|---|---|---|---|
| FDA-Approved Prescription Medications | FDA Phase I-III trials (3,000-5,000 participants) | Extensive clinical data, documented side effects | Moderate to High | Requires medical supervision, clear contraindications, established dosing |
| Established OTC Supplements (GRAS) | Dietary Supplement Health and Education Act | Decades of post-market research and widespread use | Low to Moderate | No pre-market testing, but safety accumulated through use (caffeine, omega-3s, L-theanine) |
| Newer/Lesser-Known Supplements | Dietary Supplement Health and Education Act | Limited human studies, mostly small trials | Moderate | Burden of proof on FDA to demonstrate harm, quality control varies |
| Unregulated Synthetic Compounds | Legal gray area, often imported | Minimal or no human safety data | High/Unknown | No quality control standards, long-term effects unknown, anecdotal evidence only |
In the middle range, you'll find dietary supplements with GRAS (Generally Recognized as Safe) status or extensive research backing, caffeine, L-theanine, omega-3 fatty acids, and creatine fall here. These compounds have safety records spanning decades, though they still carry potential side effects and interactions worth understanding. The FDA doesn't approve supplements before marketing, but manufacturers bear legal responsibility for ensuring safety (according to FDA guidance on dietary supplements).
At the far end of the spectrum lie unregulated synthetic compounds like racetams (piracetam, aniracetam, noopept) and novel peptides. These substances often lack human safety studies beyond small trials, creating uncertainty about long-term effects, optimal dosing, and interaction risks. The absence of safety data doesn't automatically mean danger, but it does mean you're accepting unknown risks.
The Safety Spectrum: From FDA-Approved to Unregulated
FDA-approved prescription nootropics undergo Phase I through Phase III clinical trials before reaching patients, a process that typically involves 3,000-5,000 participants over 6-7 years. This testing identifies common side effects, serious adverse events, and populations who should avoid the medication. Methylphenidate (Ritalin), for instance, carries clear warnings about cardiovascular risks and is contraindicated in patients with certain heart conditions.
Dietary supplements operate under the Dietary Supplement Health and Education Act of 1994, which places the burden of proof on the FDA to demonstrate harm rather than requiring manufacturers to prove safety beforehand. This means supplements reach consumers without pre-market safety testing. Well, established supplements like fish oil have accumulated safety evidence through post-market research and widespread use, but newer compounds haven't.
Unregulated nootropics occupy a legal gray area, not approved as drugs, not sold as supplements in the US, often imported from overseas manufacturers. Quality control varies wildly, and you're relying entirely on independent research and anecdotal reports for safety information.
Why Age Matters: Safety Considerations for Adults 55+
Adults over 55 metabolize substances differently than younger populations due to age-related changes in liver and kidney function. Drug half-lives extend, meaning compounds remain active in your system longer, potentially increasing side effect risk. A dose that causes mild jitters in a 30-year-old might produce significant anxiety in someone 60.
Polypharmacy, taking multiple medications simultaneously, becomes increasingly common with age. The average adult over 65 takes 4-5 prescription medications, each representing a potential interaction point with nootropics. Ginkgo biloba's antiplatelet effects become particularly concerning when you're already taking warfarin or aspirin (according to Cochrane systematic reviews on ginkgo).
Age-related conditions create additional contraindications. Stimulant nootropics that might be relatively safe for healthy younger adults pose cardiovascular risks for those with hypertension, arrhythmias, or coronary artery disease, conditions affecting roughly 70% of adults over 65.
Prescription Nootropics: FDA-Regulated Cognitive Enhancers
Prescription nootropics benefit from the most rigorous safety evaluation of any category. These medications must demonstrate both efficacy and safety through controlled trials before FDA approval, then continue monitoring for adverse events after reaching market. However, safety profiles established for approved uses don't automatically transfer to off-label cognitive enhancement in healthy individuals.
The distinction between on-label and off-label use matters significantly for safety assessment. Donepezil's safety profile in Alzheimer's patients, who have compromised cholinergic systems, may not predict its effects in neurologically healthy adults. Most prescription nootropics used for enhancement lack long-term safety data in non-patient populations.
Medications for Cognitive Decline: Safety Track Record
Donepezil (Aricept), memantine (Namenda), and rivastigmine (Exelon) carry FDA approval for treating Alzheimer's disease and related dementias, with safety data from trials involving tens of thousands of patients over multiple years. Donepezil's most common side effects include nausea (11% of patients), diarrhea (10%), and insomnia (9%), typically emerging at standard 5-10mg doses.
These cholinesterase inhibitors work by preventing acetylcholine breakdown, increasing this neurotransmitter's availability at synapses. The mechanism creates predictable side effects related to excessive cholinergic activity, gastrointestinal upset, muscle cramps, and bradycardia (slowed heart rate). Patients require monitoring for cardiac conduction abnormalities, particularly those with existing heart conditions.
Memantine operates differently, blocking NMDA receptors to prevent glutamate-mediated excitotoxicity. Its side effect profile differs accordingly: dizziness (7%), headache (6%), and confusion (6%) in clinical trials. The safety record for approved uses is well-established, but using these medications without cognitive impairment lacks supporting safety evidence.
Stimulant Nootropics: Higher Risk Profile
Modafinil, methylphenidate, and amphetamines carry more significant safety concerns due to their stimulant properties and cardiovascular effects. Modafinil increases heart rate by an average of 3-5 beats per minute and can elevate blood pressure, creating risks for individuals with hypertension or cardiac arrhythmias (according to a 2015 systematic review in European Neuropsychopharmacology).
A meta-analysis examining modafinil for cognitive enhancement in healthy adults found headache in 23% of participants and nausea in 11%, with most studies using single 200mg doses. Long-term safety data for cognitive enhancement purposes remains limited, the majority of trials lasted only days or weeks rather than months or years.
Methylphenidate and amphetamines carry established addiction potential, classified as Schedule II controlled substances. These medications increase dopamine and norepinephrine signaling, producing cardiovascular stress that can trigger hypertensive crises, arrhythmias, or even sudden cardiac death in susceptible individuals. Adults over 55 with any cardiovascular history should avoid these compounds unless under close medical supervision for approved indications.
Over-the-Counter Nootropic Supplements: What Science Says About Safety
OTC nootropic supplements span a wide safety range depending on the compound, dose, and individual factors. Some supplements like omega-3 fatty acids have safety records rivaling prescription medications due to extensive research and widespread consumption. Others like novel mushroom extracts lack human safety data beyond small preliminary trials.
The lack of FDA pre-market approval means supplement safety relies on post-market surveillance, independent research, and manufacturer integrity. This creates inconsistency, reputable manufacturers conduct safety testing and quality control, while others cut corners.
Natural Doesn't Always Mean Safe: Common Misconceptions
The assumption that plant-derived or "natural" supplements carry inherent safety advantages lacks scientific foundation. Ginkgo biloba, derived from ancient trees and used in traditional medicine for centuries, inhibits platelet-activating factor and can increase bleeding risk when combined with anticoagulants. This represents a serious safety concern, not a benign natural remedy.
Herbal supplements contain complex mixtures of bioactive compounds, each with potential effects and interactions. St. John's wort, sometimes used for mood and cognition, induces cytochrome P450 enzymes that metabolize roughly 50% of prescription medications, potentially reducing their effectiveness. Natural origin provides no immunity from pharmacological activity or side effects.
Quality variability compounds safety concerns with natural supplements. A 2015 investigation using DNA barcoding found that 59% of herbal supplements tested contained plant species not listed on labels, with some containing fillers or contaminants. When you can't verify what's actually in the bottle, assessing safety becomes impossible.
The Most Studied Supplements: Safety Evidence
Omega-3 fatty acids (EPA and DHA) have accumulated extensive safety data through cardiovascular research spanning decades. Doses up to 3-4 grams daily show good tolerability in most individuals, with mild gastrointestinal effects and fishy aftertaste representing the primary complaints. Higher doses may increase bleeding time, though clinical significance remains debated (according to systematic reviews in the American Journal of Clinical Nutrition).
Caffeine represents perhaps the most thoroughly studied nootropic, consumed by billions daily for over a century. Safety thresholds are well-established: up to 400mg daily for healthy adults produces minimal adverse effects, while doses exceeding 500-600mg increase anxiety, sleep disruption, and cardiovascular stress. Individual tolerance varies based on CYP1A2 enzyme genetics, which control caffeine metabolism rates.
L-theanine, an amino acid from tea leaves, demonstrates excellent safety in trials using 200-400mg doses. No serious adverse events emerged in studies lasting up to 8 weeks. Creatine monohydrate, extensively researched for athletic performance, shows similar safety at 3-5 grams daily over periods extending to five years, with no evidence of kidney or liver damage in healthy individuals.
Bacopa monnieri has safety data from trials lasting 12-24 weeks using standardized extracts (typically 300-450mg daily). Gastrointestinal side effects occur in roughly 20% of users but typically resolve with continued use or dose reduction (according to a 2021 systematic review). Theoretical concerns about thyroid function warrant caution in individuals with thyroid disorders.
Supplements with Limited Safety Data
Lion's mane mushroom (Hericium erinaceus) has entered the nootropic market with minimal human safety research. Most studies involved small sample sizes (under 50 participants) for short durations (8-16 weeks), insufficient for detecting uncommon adverse events or long-term effects.
Racetams including piracetam, aniracetam, and noopept lack FDA approval in the United States and have limited Western research. Most safety data comes from Eastern European and Russian studies with methodological limitations. Without large-scale, long-term trials, you're accepting unknown risk profiles when using these compounds.
Critical Safety Risks: Drug Interactions and Contraindications
Drug interactions represent the most serious safety concern for adults taking prescription medications alongside nootropics. The average adult over 55 takes multiple medications, each metabolized through specific liver enzyme pathways that nootropics may affect. Some interactions reduce medication effectiveness, while others amplify effects to dangerous levels.
Common Drug Interactions and Age-Related Safety Concerns
| Nootropic Type | High-Risk Drug Interactions | Age 55+ Concern | Affected Population |
|---|---|---|---|
| Stimulant Nootropics (methylphenidate, modafinil) | Cardiovascular medications, SSRIs, MAOIs | Extended half-life, increased jitters/anxiety, cardiovascular stress | ~70% of adults 65+ with hypertension, arrhythmias, or CAD |
| Ginkgo Biloba | Warfarin, aspirin, other antiplatelet agents | Increased bleeding risk due to antiplatelet effects | Older adults on anticoagulation therapy |
| Caffeine + L-theanine | Beta-blockers, some anxiety medications | Altered metabolism, prolonged stimulant effects | Adults with arrhythmias or anxiety disorders |
| Racetams (piracetam, aniracetam) | Unknown interactions (limited data) | Unclear metabolism in older adults | All populations, especially those on multiple medications |
Cardiovascular Medication Interactions
Stimulant nootropics including caffeine (above 200mg), modafinil, and methylphenidate can reduce the effectiveness of blood pressure medications by increasing sympathetic nervous system activity. This creates a pharmacodynamic opposition, your medication tries to lower blood pressure while the stimulant raises it. The net effect becomes unpredictable and potentially dangerous.
Ginkgo biloba's antiplatelet effects compound the action of blood thinners like warfarin, clopidogrel (Plavix), and even daily aspirin. This increases bleeding risk, particularly concerning for older adults already at elevated risk for falls and intracranial hemorrhage. Several case reports document serious bleeding events in patients combining ginkgo with anticoagulants.
Omega-3 fatty acids at doses exceeding 3 grams daily may also increase bleeding time, though clinical significance remains controversial. Conservative medical guidance suggests limiting fish oil supplementation to 2 grams daily when taking anticoagulants, or consulting with your prescribing physician before combining them.
Neurological and Psychiatric Medication Interactions
Combining nootropics affecting serotonin with SSRIs (selective serotonin reuptake inhibitors) or SNRIs creates serotonin syndrome risk. While rare, this condition can be life-threatening, characterized by agitation, confusion, rapid heart rate, and elevated body temperature. Rhodiola rosea and St. John's wort both affect serotonin signaling and shouldn't be combined with antidepressants without medical supervision.
Cholinesterase inhibitors like donepezil interact with anticholinergic medications commonly prescribed for overactive bladder, allergies, or sleep. These drugs work in opposite directions, one increases acetylcholine while the other blocks it, potentially canceling therapeutic effects.
Sedating nootropics including L-theanine and magnesium may enhance the effects of benzodiazepines, sleep medications, or alcohol. While L-theanine's calming effects are generally mild, combining multiple GABAergic substances can produce excessive sedation, impaired coordination, or respiratory depression in extreme cases.
When Nootropics Are Not Safe: Medical Contraindications
Cardiovascular disease represents an absolute contraindication for stimulant nootropics. Modafinil, methylphenidate, and high-dose caffeine increase cardiac workload through elevated heart rate and blood pressure, potentially triggering angina, arrhythmias, or myocardial infarction in susceptible individuals.
Kidney disease alters drug clearance, causing medications and supplements to accumulate to potentially toxic levels. Creatine, while safe in healthy individuals, requires careful consideration in those with compromised renal function due to theoretical concerns about increased kidney workload.
Seizure disorders create contraindications for several nootropics. Ginkgo biloba has been associated with seizures in case reports, possibly due to its effects on GABA neurotransmission. Stimulants can lower seizure threshold, increasing risk in epilepsy patients.
Psychiatric conditions including bipolar disorder, schizophrenia, and severe anxiety disorders may worsen with certain nootropics. Stimulants can trigger manic episodes in bipolar patients, while compounds affecting dopamine or serotonin may destabilize carefully managed psychiatric conditions.
Quality and Purity: The Hidden Safety Issue in Supplements
Supplement quality represents a critical but often overlooked safety factor. Unlike prescription medications manufactured under strict Current Good Manufacturing Practice (cGMP) regulations with batch testing and quality verification, supplement quality varies dramatically between manufacturers. What's listed on the label may not match what's actually in the capsule.

Independent testing by organizations like ConsumerLab, NSF International, and USP (United States Pharmacopeia) reveals concerning quality issues across the supplement industry. A 2019 analysis found that 22% of supplements tested contained less than 80% of the labeled ingredient amount, while 12% contained unlisted ingredients including potential contaminants.
Third-Party Testing: Your Safety Net
Third-party certification provides independent verification that supplements contain what labels claim without harmful contaminants. NSF Certified for Sport, USP Verified, and ConsumerLab testing represent the gold standard for supplement quality assurance.
Look for specific certifications rather than vague "quality tested" claims on labels. NSF certification verifies that products contain labeled ingredients at stated potencies (±10%) and are free from over 270 banned substances. USP verification includes similar testing plus manufacturing facility audits. These certifications cost manufacturers money, which is why budget supplements rarely carry them.
ConsumerLab operates differently, purchasing supplements anonymously and publishing test results publicly. Their reports identify products that fail quality standards, providing valuable information for consumers. Subscription costs around $36 annually and grants access to thousands of product reviews across supplement categories.
Standardization and Bioavailability Concerns
Herbal supplement standardization matters significantly for both efficacy and safety. Bacopa monnieri extracts standardized to 20-50% bacosides have demonstrated effects in research, while non-standardized products contain unpredictable amounts of active compounds. This variability affects both whether the supplement works and what side effects might occur.
Bioavailability, the percentage of an ingested compound that reaches systemic circulation, varies based on formulation. Curcumin, the active compound in turmeric, has notoriously poor bioavailability (less than 1% absorption), leading manufacturers to create enhanced formulations using piperine or liposomal delivery. These formulations increase absorption but may also increase side effect risk.
Storage and Expiration: Often Ignored Safety Factors
Improper storage degrades supplement potency and potentially creates harmful breakdown products. Omega-3 supplements are particularly vulnerable to oxidation, which produces rancid oils containing harmful lipid peroxides. Refrigeration after opening extends shelf life and preserves quality.
Expiration dates on supplements represent manufacturer guarantees of potency until that date when stored properly. After expiration, active ingredient content may fall below labeled amounts, though this typically represents an efficacy issue rather than safety concern. However, some compounds develop harmful breakdown products over time, particularly when exposed to heat, light, or moisture.
Side Effects and How to Minimize Risks
Even safe nootropics produce side effects in some individuals. Understanding common adverse effects, their mechanisms, and mitigation strategies helps you use nootropics more safely. Most side effects are dose-dependent, meaning they worsen with higher doses and improve with reduction.
Individual variation in side effect susceptibility stems from genetic differences in drug metabolism, neurotransmitter receptor density, and baseline neurochemistry. What causes headaches in one person may produce no effects in another.
Common Side Effects by Category
Stimulant nootropics including caffeine, modafinil, and methylphenidate commonly cause anxiety, jitteriness, increased heart rate, and sleep disruption. These effects result from enhanced sympathetic nervous system activity and increased catecholamine signaling. Timing doses earlier in the day (before noon) minimizes sleep interference, while pairing caffeine with L-theanine reduces jitters in many users.
Cholinergic nootropics like Alpha-GPC, citicoline, and huperzine A can produce headaches in roughly 15-20% of users, likely due to excessive acetylcholine activity. Starting with lower doses (Alpha-GPC at 150mg rather than 300-600mg) and gradually increasing allows tolerance to develop.
Gastrointestinal effects including nausea, diarrhea, and stomach discomfort occur frequently with bacopa monnieri, fish oil, and magnesium. Taking these supplements with food typically reduces GI side effects. For omega-3s, freezing capsules before consumption can minimize fishy burps and reflux.
Adaptogenic herbs like rhodiola rosea and ashwagandha occasionally cause mild sedation or, paradoxically, restlessness in some individuals. These opposing effects likely reflect individual differences in HPA axis regulation and stress response patterns.
The Importance of Cycling and Tolerance
Continuous use of certain nootropics leads to tolerance development, where increasing doses become necessary to achieve the same effects. Caffeine tolerance develops within 1-2 weeks of daily use, reducing its cognitive benefits while maintaining dependence. Cycling caffeine (5 days on, 2 days off, or periodic week-long breaks) preserves sensitivity.
Some nootropics like omega-3 fatty acids and creatine work through nutrient repletion rather than acute pharmacological effects, making cycling unnecessary. These compounds require continuous use to maintain tissue saturation levels that support cognitive function.
Start Low, Go Slow: Dose Escalation Strategy
Beginning with the minimum effective dose and increasing gradually allows you to identify your personal tolerance threshold while minimizing side effect risk. This approach also helps distinguish between placebo effects and genuine compound effects. For most nootropics, starting at 50% of the recommended dose for 3-5 days before increasing proves prudent.
Single-ingredient supplements before stacks helps isolate which compounds produce benefits versus side effects. If you start with a 5-ingredient nootropic stack and experience headaches, identifying the culprit becomes impossible.
Keeping a simple log tracking doses, timing, effects, and side effects provides valuable data for optimization. Note sleep quality, mood, focus, and any adverse effects daily. Patterns emerge over 2-3 weeks that aren't apparent day-to-day, helping you identify which nootropics work for you and which don't.
Making a Safe Decision: Your Nootropic Safety Checklist
Safe nootropic use requires systematic evaluation rather than impulse purchases based on marketing claims. This checklist provides a framework for assessing whether a specific nootropic makes sense for your situation, considering your health status, medications, and risk tolerance.
I kept a detailed spreadsheet for six weeks when I first started experimenting with L-theanine and caffeine combinations, tracking my 200mg caffeine/100mg L-theanine morning dose alongside sleep metrics from my Oura ring and subjective focus ratings every afternoon. Around day 18, I noticed a clear pattern: the combo worked brilliantly Monday through Thursday, but Friday doses correlated with restless sleep that night—likely because accumulated sleep debt throughout the week made me more sensitive to even morning caffeine. That log convinced me to skip Friday dosing entirely, a decision I never would have made based on how I felt on any single day.
Before Starting Any Nootropic
Consult your physician if you take prescription medications, have chronic health conditions, or are over 55. This isn't mere legal disclaimer language, drug interactions and contraindications represent real risks that your doctor can help evaluate based on your complete medical history. Bring the specific supplement with dosing information to your appointment.
Research the specific compound using primary sources like PubMed rather than relying solely on manufacturer websites or affiliate marketing sites. Look for systematic reviews and meta-analyses rather than single studies. Check whether research used the same dose and formulation you're considering, and whether studies involved healthy adults or patient populations.
Verify third-party testing for your chosen product. Search ConsumerLab's database, look for NSF or USP certification seals, or contact the manufacturer requesting Certificates of Analysis (CoA) for recent batches. Reputable manufacturers provide this documentation readily, while evasive responses signal quality concerns.
Assess your baseline cognitive function honestly. If you're sleep-deprived, sedentary, eating poorly, or highly stressed, nootropics won't compensate for these fundamental issues. Addressing sleep, exercise, nutrition, and stress management first often produces larger cognitive gains than any supplement.
Monitoring and Adjustment
Establish measurable outcomes before starting. Vague goals like "better focus" make it impossible to determine whether a nootropic works. Specific metrics, completing work tasks 20% faster, reading comprehension scores, or working memory tests available online, provide objective feedback.
Plan a trial period of 4-8 weeks for most nootropics. Some compounds like bacopa require 8-12 weeks to produce effects, while others like caffeine work within 30 minutes. Understanding expected timelines prevents premature conclusions about efficacy.
Monitor for side effects weekly using a structured approach. Rate sleep quality, energy levels, mood, and any physical symptoms on a 1-10 scale. Subtle changes become apparent when tracked systematically versus relying on memory.
Discontinue immediately if serious side effects occur, chest pain, severe headache, difficulty breathing, significant mood changes, or allergic reactions. These warrant medical evaluation rather than "pushing through" hoping they'll resolve.
Red Flags: When to Avoid a Nootropic
Avoid products making disease treatment claims. Legitimate supplements can't legally claim to "cure Alzheimer's" or "treat ADHD", such claims indicate either illegal marketing or outright fraud. The FDA warning letters database lists companies making prohibited claims.
Be skeptical of proprietary blends that hide individual ingredient doses. These formulations prevent you from knowing whether you're getting effective amounts of active compounds or mostly filler. They also make it impossible to identify which ingredient caused side effects if they occur.
Question products with unrealistic claims or no cited research. If manufacturers can't provide published studies supporting their product (not just testimonials), that's a significant red flag. Well, extraordinary claims require extraordinary evidence.
"When a product doesn't disclose the amount of each ingredient, you have no way to assess safety or effectiveness—it's essentially asking consumers to trust blindly," says Dr. Pieter Cohen, Associate Professor of Medicine at Harvard Medical School and researcher specializing in dietary supplement safety.
Nootropic safety ultimately depends on informed decision-making rather than blind trust in marketing claims or regulatory oversight. The supplement industry operates with minimal pre-market safety requirements, placing responsibility on you to research compounds, verify product quality, assess interactions with your medications, and monitor effects systematically. By understanding the safety spectrum from prescription medications to unregulated compounds, recognizing your individual risk factors, and following a methodical approach to evaluation and use, you can make reasoned decisions about whether specific nootropics align with your health goals and risk tolerance.
Related Articles
- Nootropic Supplements: What Are They and How Do They Work?
- L-Theanine Side Effects: Safety Profile and Contraindications
- Complete Nootropic Supplements List: All Compounds Explained
- Best Nootropic Dietary Supplements: Evidence-Based Rankings
- Nootropics vs Regular Supplements: Understanding the Difference
- L-Theanine Dosage Guide: How Much to Take for Anxiety and Focus
Frequently Asked Questions
What's the difference between prescription nootropics and over-the-counter supplements in terms of safety?
Prescription nootropics like modafinil undergo rigorous FDA testing with 3,000-5,000 participants before approval, providing extensive safety data and clear dosing guidelines. OTC supplements lack pre-market FDA testing but may have decades of post-market safety data if they're established compounds like caffeine or omega-3s. Prescription medications carry documented side effects and contraindications, while supplement safety varies widely depending on the specific compound.
Is 'natural' the same as 'safe' when it comes to nootropic supplements?
No. Natural ingredients can still carry significant risks, cause side effects, and interact with medications. Safety depends on the specific compound, your health status, dosage, and current medications—not whether something is natural or synthetic. Even well-studied natural supplements like omega-3s can interact with blood thinners or cause side effects at high doses.
What should I do before starting any nootropic supplement?
Consult your doctor about your current medications and health conditions to identify potential interactions and contraindications. Start with the lowest recommended dose and increase gradually ("start low, go slow"). Choose products with third-party testing certification to ensure quality and purity, and monitor yourself for side effects or adverse reactions.
Which nootropic supplements have the most safety evidence?
Caffeine, L-theanine, omega-3 fatty acids, and creatine have the strongest safety records with decades of research and widespread use. These compounds have established dosing guidelines, known side effect profiles, and extensive post-market data. Newer or lesser-known supplements typically have limited human studies and moderate risk levels due to insufficient safety data.
What are red flags that I should avoid a particular nootropic?
Avoid nootropics if you have contraindications based on your medical history, take medications that could interact with them, or if the product lacks third-party testing or quality certification. Also be cautious with unregulated synthetic compounds that lack human safety studies, and stop use immediately if you experience cardiovascular symptoms, severe headaches, or psychiatric changes.
How do I know if a nootropic supplement is actually safe and pure?
Look for third-party testing certifications from organizations like NSF International or USP, which verify that products contain what they claim and are free from contaminants. Check for standardization information on the label and verify the manufacturer's reputation. Also review storage conditions and expiration dates, as improper storage can degrade safety and efficacy.
Can I take multiple nootropics together safely?
Combining nootropics increases the risk of unexpected interactions and side effects, especially if you're also taking medications. Before stacking supplements, consult your doctor about potential interactions between specific compounds. Start with single nootropics first to establish your tolerance and response before considering combinations.
What does 'cycling' nootropics mean and why is it important?
Cycling means taking breaks from nootropic use to prevent tolerance buildup and allow your body to reset. For example, you might take a supplement for 5 days, then take 2 days off. This strategy helps maintain effectiveness and reduces the risk of dependence or diminishing returns, though specific cycling protocols depend on the individual nootropic.




